Understanding and Managing Childhood Eczema
What is Childhood eczema?
Child and eczema (Childhood eczema), also known as atopic dermatitis, is a common chronic skin condition that affects many children worldwide. It is characterized by dry, itchy, and inflamed skin, often leading to discomfort and distress for both the child and their caregivers. In this article We will explore the causes, symptoms, triggers, treatment options, and practical tips to help parents and caregivers navigate this condition, ensuring the best possible care for children with eczema.
Understanding about Childhood Eczema (Symptoms and Sign)
The symptoms of child eczema (atopic dermatitis) can vary from mild to severe and may include:
Dry and sensitive skin
The skin may feel rough, scaly, or flaky.
Itching
Itching is a common symptom of eczema and can be intense, leading to scratching, which can further worsen the condition.
Redness and inflammation
Affected areas of the skin may appear red, swollen, and irritated.
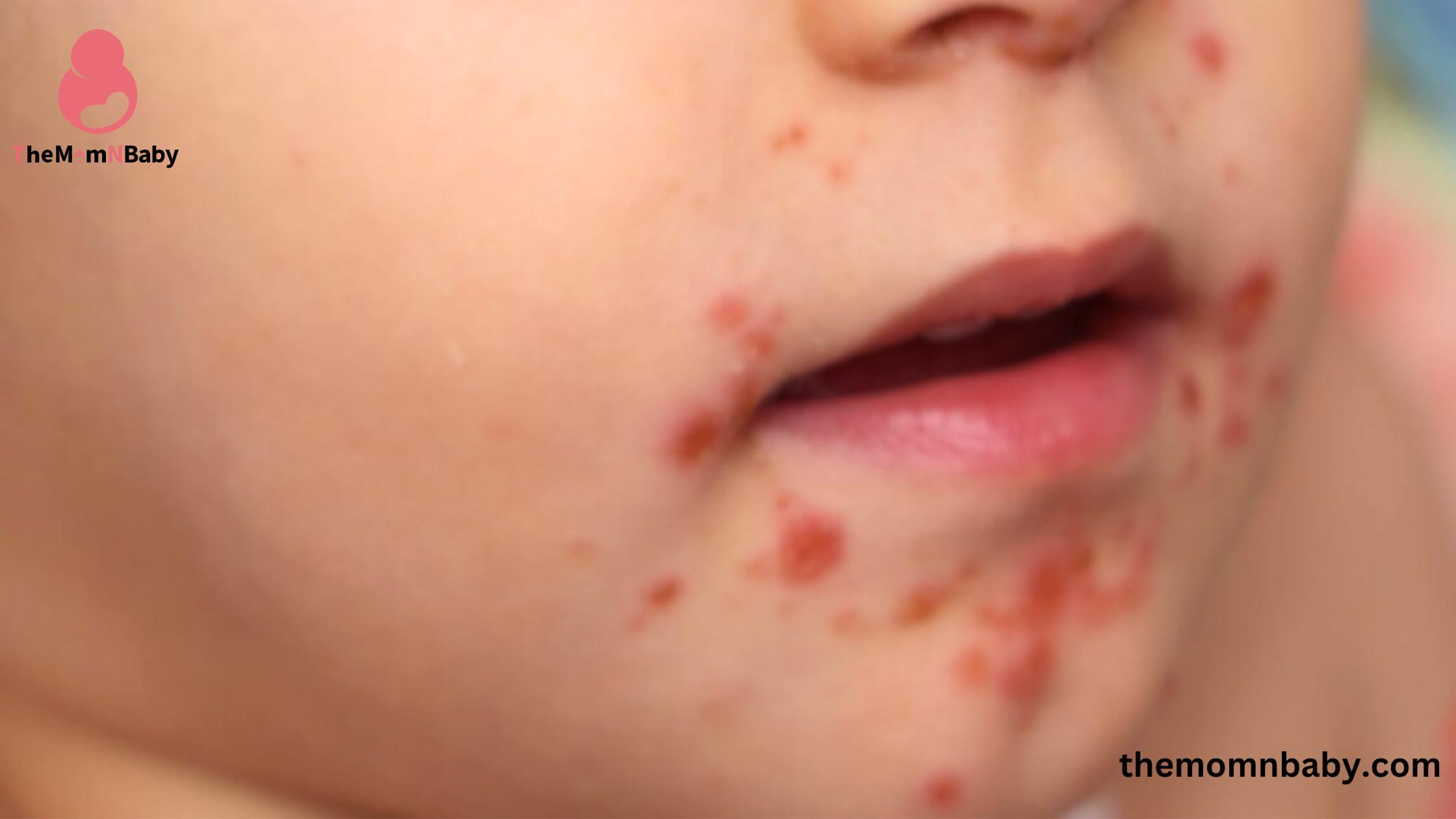
Rashes or patches
Eczema typically presents as red, raised rashes or patches on the skin. These patches may be rough, thickened, or crusty.
Cracked or weeping skin
In severe cases, the skin can become cracked, open, or oozing fluid, making it susceptible to infections.
Skin discoloration
Over time, the affected areas may become darker or lighter in color than the surrounding skin.
Sleep disturbances
Itchiness and discomfort can disrupt sleep patterns, leading to fatigue and irritability.
Emotional impact
Child eczema can cause emotional distress, impacting a child’s self-esteem and overall well-being.
It is important to note that eczema symptoms can fluctuate, with periods of flare-ups and remission. The severity and frequency of symptoms may vary from child to child. If you suspect your child has eczema or notice any of these symptoms, it is advisable to consult a healthcare professional for an accurate diagnosis and appropriate management strategies.
What is the reason for eczema? / Causes of child eczema
The causes of child eczema (atopic dermatitis) are not fully understood, but it is believed to involve a combination of genetic, immune system, and environmental factors. Here are some key causes and contributing factors:
Genetic Predisposition:
Eczema tends to run in families, indicating a genetic predisposition. Children with a family history of eczema, asthma, or allergies are more likely to develop the condition.
Immune System Dysfunction:
Children with eczema have an overactive immune response, leading to inflammation and skin barrier dysfunction. This makes the skin more susceptible to irritants, allergens, and infections.
Skin Barrier Dysfunction:
The skin of children with eczema has a weakened protective barrier, allowing moisture to escape and irritants to penetrate. This leads to dryness, sensitivity, and susceptibility to triggers.
Environmental Triggers:
Various environmental factors can trigger or worsen eczema symptoms. These triggers can include irritants like harsh soaps, detergents, and chemicals, as well as allergens such as dust mites, pet dander, pollen, and certain foods.
Allergies:
Children with eczema are more likely to have allergies, such as food allergies or allergic rhinitis. Allergens can trigger an immune response that worsens eczema symptoms.
Climate and Weather
Extreme weather conditions, such as cold, dry winters or hot, humid summers, can aggravate eczema symptoms. Changes in temperature and humidity levels can cause dryness and itchiness.
Stress and Emotional Factors
Emotional stress, anxiety, and frustration can trigger or exacerbate eczema symptoms. Stress management techniques and addressing emotional well-being are important in managing the condition.
Irritating Substances
Certain substances can irritate the skin and trigger eczema flare-ups. These can include synthetic fragrances, harsh soaps, detergents, and fabrics like wool or rough materials.
What are the triggers for eczema flare-ups, and can we prevent them using specific strategies?
Triggers and prevention strategies play a crucial role in managing and preventing eczema flare-ups in children. By identifying and avoiding triggers, parents and caregivers can help minimize the impact of eczema on their child’s skin. Here are some common triggers and prevention strategies:
Allergens:
- Food Allergens: Identify and avoid any specific foods that may trigger eczema flare-ups in your child. Consult with a healthcare professional or allergist to conduct allergy testing if necessary.
- Environmental Allergens: Reduce exposure to common environmental allergens such as dust mites, pet dander, pollen, and mold. Regular cleaning, using allergen-proof covers for bedding, and keeping pets out of the child’s bedroom can help minimize exposure.
Irritants:
- Harsh Soaps and Detergents: Use gentle, fragrance-free soaps, cleansers, and detergents that are suitable for sensitive skin. Avoid products that contain irritants such as sulfates and synthetic fragrances.
- Chemical Irritants: Minimize exposure to harsh chemicals, such as household cleaning products and certain fabrics. Opt for natural and hypoallergenic alternatives whenever possible.
Climate and Weather:
- Dry Climate: In dry climates, it is important to maintain proper moisture levels in the skin. Use a humidifier to add moisture to the air in your home, and regularly moisturize your child’s skin to prevent dryness.
- Hot and Humid Weather: During hot and humid weather, keep your child’s skin cool and dry. Dress them in loose, breathable clothing and use lightweight bedding.
Stress and Emotional Factors:
- Stress Management: Help your child manage stress through activities such as relaxation exercises, mindfulness, and engaging in hobbies or activities they enjoy.
- Emotional Support: Provide emotional support and create a nurturing environment for your child, as emotional stress can trigger eczema flare-ups.
Skin Care:
- Moisturize Regularly: Apply a fragrance-free moisturizer to your child’s skin at least twice a day, especially after bathing, to help maintain skin hydration and prevent dryness.
- Gentle Bathing Practices: Use lukewarm water for baths and limit bath time to 10-15 minutes. Avoid using harsh soaps and opt for mild, fragrance-free cleansers designed for sensitive skin.
- Pat Dry: After bathing or washing, gently pat your child’s skin dry with a soft towel. Avoid rubbing, as it can further irritate the skin.
Clothing and Fabrics:
- Choose Soft Fabrics: Dress your child in loose-fitting, soft fabrics like cotton. Avoid wool and synthetic materials that can cause irritation and trigger eczema flare-ups.
- Wash New Clothes: Wash new clothes before your child wears them to remove any potential irritants or chemicals.
Allergy Management:
- Identify Allergies: Work with healthcare professionals to identify and manage any underlying allergies that may contribute to eczema flare-ups.
- Allergy-Proof the Home: Take steps to minimize exposure to allergens by keeping the home clean, using air purifiers, and regularly washing bedding in hot water.
Managing Childhood Eczema: Practical Tips
A. Skincare Routine
- Gentle bathing practices
- Moisturizing techniques and products
- Choosing suitable skincare products
B. Clothing and Fabric Choices
- Breathable and soft fabrics
- Avoiding rough or irritating materials
- Dressing for different weather conditions
C. Itch Management
- Nail care and scratch prevention
- Cooling techniques (wet wraps, cool compresses)
- Distraction and relaxation techniques
D. Diet and Nutrition
- Identifying and managing food triggers
- Nutritional considerations for healthy skin
- Consultation with healthcare professionals
E. Medical Treatment Options (topical and systemic)
- Topical Corticosteroids and Other Medications: These are applied directly to the skin to reduce inflammation and relieve itching.
- Immunomodulators and Barrier Repair Creams: These help modify the immune response and improve the skin barrier function.
- Oral Medications in Severe Cases: In severe eczema, oral medications like antihistamines or corticosteroids may be prescribed to control symptoms.
- Allergy Testing and Immunotherapy: Identifying specific allergens through testing can guide avoidance strategies, and immunotherapy may be used to desensitize the immune system to allergens over time. These treatments are particularly relevant if allergies contribute to eczema flare-ups.
It is important to consult with a healthcare professional to determine the most appropriate treatment options for a child with eczema.
Professional Advice and Follow-up Care
- Treatment Plan: Work closely with the healthcare professional to develop a comprehensive treatment plan tailored to the child’s specific needs and the severity of their eczema.
- Regular Follow-up: Attend follow-up appointments to monitor the progress of the treatment and make any necessary adjustments.
- Medication Management: Ensure proper usage of prescribed medications, understanding their application, dosage, and potential side effects.
- Address Concerns: Discuss any concerns or questions with the healthcare professional to ensure clarity and understanding.
- Open Communication: Maintain open communication with the healthcare professional regarding any changes in symptoms, triggers, or overall well-being.
“Childhood eczema poses challenges for children and caregivers alike, but with adequate understanding and management strategies, it is possible to provide effective care and enhance the child’s quality of life. By identifying triggers, employing preventive measures, establishing a consistent skincare regimen, and seeking professional advice as necessary, parents and caregivers can assist their child in managing eczema and minimizing its impact on overall well-being. It is essential to remember that each child’s experience with eczema is unique, so patience, adaptability, and a comprehensive approach are crucial for achieving positive outcomes.”






